|

 Sign or View My Guest Book
|
11:00 p.m. - Thursday, Jun. 11, 2009
cancerblog MOVING
I've moved this blog to my site, and will be closing my diaryland account soon.
See http://www.duberweb.com/cancerblog for the latest updates.
1:30 p.m. - Saturday, Oct. 25, 2008
Two years later...
...and still cancer-free. Oncologists never use the word "cured," because there's no way to tell if cancer is in remission or gone permanently. So they would most likely say I'm in a remission period. It feels great to be back to my old self.
The PET/CT scans are now down to twice a year, and next year should be an annual test.
I wanted to again say thanks to all of those who showed their support during my treatment and recovery and didn't think cancer is as contagious as the plague - Sandi, Drew, my Mom, Amanda, Gwen, my health care professionals, the kind folks at the oncology center, those who I've thanked in my earlier posts, and many others.
I'll close the blog with three words:
Never Lose Hope.
8:59 p.m. - Monday, Jul. 10, 2006
PET Scan Results
First day back at work. I've been able to adjust to sleeping at night and had no trouble getting up early.
More great news - my scan was completely clear. No questionable areas whatsoever.
My next scan will be in October.
11:55 p.m. - Thursday, Jul. 6, 2006
PET Scan
I originally made the appointment for this PET scan for the afternoon because I'm still having trouble falling asleep at night.
I didn't find out until later that I had to fast for five hours prior to the test. Had I known, I'd have made it for early morning and forced myself out of bed.
It went okay though. I'll find out the results next Monday morning.
9:35 p.m. - Friday, Jun. 16, 2006
Oncologist Visit
Saw the oncologist today. He's okay with the decision not to have me undergo radiation therapy.
He asked me how I felt and I told him that my energy was slowly coming back, and the headaches have pretty much gone away.
My hair is starting to grow back and the only real difficulty I'm still having is sleeping at night.
He okayed me to go back to work on July 10. That sure is great news!
I need to have a final PET scan in one month and then a follow-up to discuss it.
If all looks well then he'll just monitor me with scans every three months for awhile, then every six months, then once a year.
11:08 p.m. - Tuesday, May 23, 2006
Radiology Oncologist Followup
After reviewing my latest PET scans and conferring, both of my doctors came to the conclusion that the best course to take is not to give me radiation treatment. There is not enough showing up on the scans to merit targeting any particular area. Instead they'll monitor me closely with periodic scans.
It's certainly a great relief, but I hope it really is the best course of action.
Next will be my final appointment with my oncologist, which has been rescheduled to 16 June.
2:39 p.m. - Monday, May 22, 2006
Why this blog exists
It has recently occurred to me that I had launched directly into these writings without any explanation whatsoever to my potential readers. I now feel that I owe everyone at least that courtesy.
One of the main reasons for creating this blog was to keep family, friends, and coworkers informed of my progress. Due to side effects of the chemotherapy it hasn't been as timely as I would have liked. Getting the laptop helped, especially since my desktop computer has been out of commission for about a month.
[So if you've emailed me (or not) and I haven't contacted you yet -- please email me again so that I can save your address on my laptop. My emails up to the start of May, as well as my address book, are on the desktop, still unavailable for now despite a new power supply, motherboard, processor, memory, and video card.]
Another reason for this written account is to provide myself with a historical record of the whole ordeal, with dates and treatments on file for easy reference.
But the third and perhaps most important reason is to let others know what to expect should they or someone close to them be facing the decision of whether or not to receive chemotherapy treatment.
When I made my decision, I wasn't aware of what I would be facing - and maybe that's for the best. A quote from "Coping With Chemotherapy" by Nancy Bruning struck home with me:
"The chemotherapy experience can fall short of what it might be - how it can be used, how it can benefit, and the degree of comfort the patient maintains while undergoing it - because chemotherapy patients suddenly find themselves plunged into a maze without a map. Cancer care for most people is completely foreign territory - full of half-truths, myths, and misconceptions, of personal issues and dilemmas, of complicated new words and procedures, of hot and cold running hope and fear."
That statement was written in 1985 and unfortunately is still true over 20 years later.
My hope is that this blog will be forwarded to those who are facing chemotherapy, have already started it, or have loved ones who are facing or have already started chemo.
That it will help them in some small way, to know a little better what to expect, in addition to what their doctors tell them. The doctors can't tell you everything. I knew a little more from what friends and other survivors could tell me, but if you haven't lived through it yourself, you can't relate it to anyone else.
So among my next posts will be a retelling of how this ordeal has affected me, mainly physically. The psychological effects obviously vary from person to person, so I may not have much to say about that, aside from how support from friends and family has helped.
I won't be relating what symptoms others have related to me if I haven't experienced them myself. I can only say what has happened to me personally.
12:41 a.m. - Saturday, May 20, 2006
Thank You's
Follow me, don�t follow me
I�ve got my spine, I�ve got my orange crush
-- R.E.M.
No more chemo, no more orange crush. Or tang, or whatever you want to call the Red Devil's (Doxorubicin) side effects...another thing I won't miss.
I seem to be back to where I'm sleeping a lot (except at night) and am sore all over. My last blood cell counts were higher than they've been since I started chemo, so it's not anemia. Maybe I have to go back through the cycle backwards before returning to my old self.
I wanted to say thanks to members of my family who have been supportive, as well as friends, coworkers, and total strangers. Special thanks to Mike S., Danny R., Larry F., Manda, and Gwen.
Thanks for the emails even though I haven't gotten around to answering them (sorry!). Thanks to Diana G., Barb, Rose, and others for the cards. Every kind word is read and taken to heart.
No man is an island - a hermit perhaps, but not an island. I wouldn't be where I am today without the prayers and positive thoughts of others, added to my own. Collectively it has a powerful effect.
The person I have to thank the most is the most caring and selfless person I've ever met. She manages my appointments as well as making sure I get out of bed in time and driving me to them, which takes a lot of things off my mind so I can rest, but unfortunately places a lot of burden upon her. And she's not only doing all this for me, but for her father as well, who is going through health problems of his own right now. And never once have I heard one word of complaint. Sandi, you're the greatest.
Thanks again to all. I may not have mentioned everyone, but if you've contacted me, you know who you are.
10:37 p.m. - Tuesday, May 16, 2006
Scan Results
After last week's period of activity, I'm back to sleeping a lot and having no energy this week. It seems to come and go. Hopefully it will do so more frequently as time goes on.
Visited my oncologist today and he said my scans were night and day compared to the last ones. However, there were still some questionable areas. I asked him what they were, and he said it's difficult to tell if active spots are due to RA inflammation or cancer. On one hand, symmetrical uptake (i.e. both hips) are probably due to RA, but random spots are usually cancer cells.
He's under the impression that I may need a minimum treatment of radiation therapy for three weeks. He'll be speaking to the radiation oncologist prior to my visit next week.
My bone density scan showed some bone thinning, so he prescribed 1200mg/day of calcium supplements, as well as 1 Fosamax per week. Also 1000 units/day of Vitamin D along with 15 minutes of sun daily.
He wants to see me again in four weeks, and to have a CAT scan in eight weeks (not CT/PET). And after all my treatment is completed, to see the cardiologist for a final 3D echo cardiogram.
He seemed to think that I should be driving myself by now, although I still experience times when a wave of exhaustion hits me so hard it's as if I lose consciousness rather than fall asleep. It can hit me at any time, but is guaranteed to happen whenever I'm out doing things for several hours. Which is why Sandi is driving me to appointments and everywhere else we go.
11:55 p.m. - Thursday, May 04, 2006
Scans
I've been having a little more energy and motivation this week and have been able to get some things done. In my lethargic periods it takes a lot of effort just to get out of bed in the morning and get myself something to eat. But I managed to do some yardwork this week and get some handyman work done inside the house.
Before the bone density scan, I had a fasting blood sugar test and my level was 92, which I'm told is normal. So that was good news. The bone density scan took place inside the faciility (as opposed to the PET scan in the trailer) and didn't take long at all. No injections.
The PET scan took much longer as they waited almost an hour for the isotopes to circulate and accumulate. But at least it was painless. I fell asleep while waiting but managed to stay awake during the whole scan. That may be a first.
My oncologist should have the results in a few days, and I can pick up my copies next week.
10:04 p.m. - Friday, Apr. 28, 2006
Radiation Oncologist
Today was my first visit with the radiation oncologist. An initial visit to review my case so the doctor may later determine if I'm a good candidate for radiation therapy. After turning in whatever scans I had and filling out the usual paperwork, it was a short wait until we saw the doctor.
She briefly examined me and asked questions as she went along. She said my underarm and pelvic lymph nodes are okay. Everything that was abnormal, according to all my scans, is getting better. My rheumatoid arthritis may have increased the side effects of my treatment, but there are fewer in cases where the RA is under control.
She seemed to have a wait-and-see attitude, but also said the preliminary diagnosis is that I may not need any radiation treatment at all.
I need to go back at least two weeks after my scans for my next visit, at which time she'll have a plan developed for my treatment. If I am to be treated, I'll be fitted with a face mask since the radiation will be mostly to the neck area, where the large tumor was. I will also undergo tests at that time and be scheduled for my first treatment.
At this point she can't say how many weeks of treatment I would need or how much radiation. Lymphoma requires less radiation than other types of cancer because it's more sensitive to it. But the treatments would be daily (Mon-Fri) for 30 minute periods. I could schedule anytime between 7:30 to 4pm.
She sent me off with a cd video, vhs tape, and hardcopy info that describe radiation treatment and side effects and should answer any questions I might have.
Her prescription for me was to get out and walk as much as possible, and enjoy quiet hobbies. On the way out I made a follow-up appointment for May 23.
10:57 p.m. - Sunday, Apr. 23, 2006
Feeling Better
Although I'm still not sleeping much at night, this weekend I had a little bit of energy. It felt great to be able to get up and do things. I plan to enjoy it while it lasts - probably until the radiation starts.
Forgot to mention that on last Tuesday, the 18th, I saw the oncology P.A. at his request. The cat had bitten me three times last Friday night/Saturday morning (14/15 April) and once again Saturday night/Sunday morning. She broke the skin so Sandi called the doctor (not to mention the veterinarian) who wanted to make sure there was no infection.
Fortunately there wasn't; it was only only a scratch. Unfortunately, the reasons behind the cat's aggression could fill a whole other blog. Let's just say we're working with the cat on this one.
More good news was that my blood cell counts were okay. I had to get a new prescription for my headaches but as they're fewer and further between I have a feeling this will be the last. Maybe this means that my energy and motivation levels will be gradually picking up soon.
11:26 p.m. - Sunday, Apr. 16, 2006
Easter Sunday
Today is Easter and I'm starting to gradually get some energy back. Friday I was able to go out to run some errands, and today was the first day I haven't spent in bed for a long time. I had a brief period of motivation and energy this afternoon; just enough to unpack and stack some boxes in the basement.
Sandi made my appointments for me, and was able to get them scheduled at the same facility on the same day. I'll have the bone and PET/CT scans on 4 May. She's really great at helping me out by making appointments and keeping track of them for me. She knows I sleep a lot during the day and sometimes don't have the energy or motivation to even get up and talk to people on the phone. Of course, I'm always glad when I do get the chance to talk to someone.
10:42 p.m. - Wednesday, Apr. 12, 2006
Blood Test Visit
I've spent the past week after chemo in bed, dozing on and off until late afternoon and unable to get back to sleep until 2 or 3 in the morning. Sunday night I felt well enough to go out for some ice cream after dinner, and actually drove for a change.
Today was a busy and tiring day with three doctor's appointments.
I first met with my rheumatologist to discuss the resumption of my treatment now that I've finished chemo. I learned that Rituxan is being looked into for treating Rheumatoid Arthritis, and the doses I've received over the past four months may keep my RA in remission for up to six months. However, Rituxan would only be used in cases where patients haven't responded to anything else.
Since I've responded well in the past to Methotrexate and Arava, we probably won't have to go back to biological response modifiers/TNF blockers like Humira and Enbrel. Which is fine with me - I've had enough needles now to last me a lifetime.
Dr. Y. is very active in the international medical community and will probably present my case at various symposiums. Not much research is available on RA patients who have been given Rituxan, so I can expect to hear from him and may be asked to tell my story in person.
At any rate, if I am to receive radiation treatment, I'm to stop the Prednisone for the duration. I'm down to 10mg/day as a maintenance dose.
Next was my oncologist, for my between-treatment appointment to check my blood counts and see how I'm doing. My white blood cell count was low but apparently not low enough to require a shot. It should start picking up but the doctor still wants me to take a Tequin for the next five days to ward off infection and prevent fever.
He asked about symptoms and side effects, and I told him aside from the usual, my legs have been very sore during the past week. Not just the joints, but in the muscles, tendons, or ligaments. He told me that was common, and the medical term was arthralgia.
A fancy name for sore joints.
He wants to see me again in about five weeks, so I made an appointment for 16 May. Prior to that, around 8 May, he wants me to get a bone density test and a final PET/CT scan. The bone density test will show if my bones have been affected by the chemotherapy medications. They can sometimes cause a loss of bone density, which in turn can cause a lot of problems. I don't know what the treatment for that would be, but I'm sure it's correctible. The PET/CT scan will show if there is any cancer left in my body.
I asked about the radiation, and he wants me to make an appointment to be evaulated for radiation therapy as soon as possible. The radiation would be mainly to the neck area, where the tumor was. I made an appointment on the way out with the radiation oncology folks for 28 April, and I need to bring with me whatever films I have of any scans or X-rays, which is not many.
The third appointment was with a dermatologist for an unrelated issue. I'm sure that Andrew was glad when we were all finished, after dragging him around all day only to spend a great deal of time in waiting rooms. He was very patient and a good sport about it all.
10:38 p.m. - Wednesday, Apr. 5, 2006
Chemo Round Eight
Today I saw the doctor's assistant (P.A.) prior to my treatment. I told him how I have absolutely no energy or motivation and mostly sit in bed or the recliner, spending a lot of time reading and sleeping.
He said I'm experiencing the "chemo blues." It usually affects patients around or after the sixth treatment. Today is my eighth and last treatment, and I've been this way for quite awhile now. The medical term for it is asthenia. A fancy name for having little or no energy or motivation.
I also asked about the radiation treatment Dr. K. had in mind, as I mentioned in my December 6th entry. He'd mentioned on two occasions that he wanted to follow up the chemotherapy with a dose of radiation. The P.A. said that radiation therapy would not be by injection, but by exposure/irradiation. It's usually daily (Mon-Fri) for 3-6 weeks, taking about 30-45 minutes each session.
Facing the treatments doesn't really bother me, but the thought of Sandi having to drive me there (at least 35 minutes each way) and then having to go to work (at least an hour each way) every weekday, concerns me a great deal. That's a lot of stress for her. Maybe by then I'll be able to stay awake at the wheel long enough to drive myself.
After speaking to the doctor I received my last chemo treatment. My white blood cell count is 7.6, up from .8 two weeks ago, so that's good news. The nurse had to stop my IV drip for awhile when I started to feel my heartrate increasing and a kind of rushing feeling in my chest. Kind of how you feel before you get nauseous. After a while I felt okay. I was glad that Sandi was able to keep me company again. She was able to catch a few moments of sleep in an empty recliner, as I did after receiving the Benadryl.
It may take six weeks or more for this final dose of drugs to be completely purged from my system. The more time that passes, the more "back to normal" I should feel.
On my next visit with Dr. K. I'll have to ask exactly what part of my body will be treated with radiation. The tumor was in my neck, but the cancer was in my lymph system both above and below the waist.
11:26 p.m. - Monday, Apr. 03, 2006
A Better Weekend
This past weekend I felt better than the last, but still didn't have much energy to do anything. This is week three since my last chemo treatment, but I'm not feeling quite as energetic as I did during my last three-week hiatus. I've had achy joints almost every day, along with occasional bouts of drowsiness. But those could be unrelated to the chemotherapy - I'll be sure to mention it on during my doctor visit this coming Wednesday.
10:07 p.m. - Wednesday, Mar. 29, 2006
2nd 2D Echo Test
I had my 2D Echo cardiogram test today. It went pretty much the same as the last one and didn't take too long. My doctor should have the results well in time for my next appointment.
Last Friday, the 24th, was my last session of Physical Therapy, so I may be able to get more things done now.
11:01 p.m. - Wednesday, Mar. 22, 2006
Labs
Had my blood checked today, with the usual results - low red and white cell counts. I wasn't given a shot of Aranesp this time, but the doctor did instruct me to take a Tequin tablet (the antibiotic) once a day for the next five days just to be on the safe side.
The side effects of treatment remain about the same, but fortunately there are no new ones. Several people have told me they lost their sense of taste after a couple of treatments, but I'm glad to say that hasn't happened to me.
6:54 p.m. - Monday, Mar. 20, 2006
The Lost Weekend
This last round of chemo has really hit me hard. I was in bed all weekend, sleeping on and off during the day, and up most of the night until three or four in the morning, resting in a recliner. I had no energy at all and felt wiped out and drowsy. I still feel that way but at least didn't sleep all day. Last night I was able to go downstairs to look for something, so my energy is slowly coming back.
Getting a laptop computer was a great decision because now I can work on this blog and my web sites, check email, and more. I just haven't been up to sitting in a chair for any length of time for a while now. It makes my legs sore for one thing, mostly in the knees. At least I feel a little more productive now, even if I'm not. And that's all that matters, anyway.
Last week was quite a week and we were on the road almost every day. In addition to having the PET scan, picking up the results the next day, and chemotherapy, I had an unrelated outpatient procedure and physical therapy for some slight nerve damage in my right shoulder resulting from the biopsy in December. That could have added to my exhaustion somewhat.
This week will be almost as busy - an appointment with my shoulder doctor, labs on Wednesday, physical therapy, and my sleep study on Saturday.
11:48 p.m. - Wednesday, Mar. 15, 2006
Chemo Cycle 7
We picked up the PET scan results yesterday and Dr. K looked at them this morning. He said they looked great, showing about 80% of the cancer is gone. He wants me to have another 2D Echo cardiogram done two weeks from now to see if my heart is strong enough to withstand another round of chemotherapy. If the results look good, the final round will be in three weeks' time.
The chemotherapy session afterwards went pretty well and only lasted about three hours. It seemed to go even quicker since Sandi was able to sit with me and keep me company. Not to mention going out to get us some real lunch food.
I have to go back for blood labs next week, then I have two weeks off again. Or no more treatments, depending on the test.
Dr. K. is also wanting to do a final treatment of radiation therapy regardless. He didn't say (and I forgot to ask) if that would be an injection of isotopes or external exposure.
11:38 p.m. - Monday, Mar. 13, 2006
Second PET Scan
Today I had my second PET scan to see how successful the chemotherapy has been. The experience wasn't nearly as bad as the last time. I didn't get nauseous and my heart wasn't racing. I felt okay afterwards and didn't have to lie in bed the rest of the day.
Having chemo every three weeks feels much better than every other week. This past week I've felt my energy returning a little as the anemia subsided. I also feel better when I can do more instead of just rest or not have the energy to do anything more than sit up in bed and read. It feels good to be able to get out and about.
Of course, Sandi is still driving me around everywhere because of my sleep disorder. I'm very fortunate to have such a loving, devoted spouse. And thankful that she can make use of the Family Leave Act to help me out.
5:16 p.m. - Thursday, Mar. 02, 2006
Mid-session Visit
Yesterday my red and white blood cell counts were low again so they gave me another shot of Aranesp. As a result I've had spasms of pain in my lower back most of the day today. Pain relievers help but they took all day to start working.
The doctor also wanted me to take Tequin once a day just as a precaution.
Since I've been going to bed late and not having energy until the afternoon, 3pm has become my 7am, when I get up and have enough energy to start doing things. It will take some adjusting before I go back to work.
12:10 p.m. - Saturday, Feb. 25, 2006
Cycle 6
This week's session was much shorter as promised - around 3-4 hours. The doctor doesn't want me to come in for another treatment until three weeks from now instead of two. So I get a week off where I may start feeling better.
He also wants me to have another PET/CT scan in about two weeks. That will show us how much more progress has been made.
The treatment made me fatigued the rest of the day Wednesday and most of Thursday and yesterday. I seem to have more energy in the afternoon after resting all day, and can do some things around the house in the evening.
1:45 p.m. - Sunday, Feb. 19, 2006
Reaction and rebound
Wednesday's shot did a number on me. I woke up Thursday morning with a sore chest and throbbing lower back pain. The muscle relaxant helped and I stayed in bed most of the day.
I felt a little better Friday and was able to get up and about. I spent most of yesterday in bed resting and felt back to "normal" by yesterday evening.
I didn't feel any need to call the doctor's office because I'd expected some sort of reaction, and it was manageable.
5:50 p.m. - Wednesday, Feb. 15, 2006
Mid-session Visit
Nothing much to report to the doctor today. I still get headaches almost daily but not severe ones. My fingertips are still a little numb but not so much that I can't use them. Today I don't have much energy at all.
One reason may be chemotherapy-related anemia - my red blood cell counts were low, with hemocrit being around 35. That compares to 36.7 last Wednesday, with 37-52 being in the normal range.
That doesn't seem much to me, but it must be enough to affect me. He had the nurse give me Aranesp by injection to help the bone marrow in my body produce more red blood cells. That should help with the anemia, which usually comes on gradually as someone undergoes more and more chemotherapy treatments.
My white blood cell count was low as usual, and should start rising in the next couple of days.
I wondered, since my red cell counts were low and my white cell counts were low, what cells are left in my blood?
I forgot to tell the doctor that my legs and joints in general have been really sore the past few days. But that may just be due to shoveling snow last Sunday.
2:59 p.m. - Saturday, Feb. 11, 2006
Cycle 5
Last Wednesday's treatment didn't wipe me out too much. No severe headaches or sleeping all day so far. Blood counts looked good, too.
The nurse said she'll indicate on my chart that the next time I should have a faster drip so it will only take about three hours instead of five. What had happened was that I'd had a different nurse administering the medications each time, and each was going by the preceding treatment, which were all five hours.
Since there was nothing in my chart saying I didn't have any adverse reactions, they erred on the safe side and assumed there was a reason for a slow drip.
Fortunately Sandi is arranging to have more time off at work through leave donations. She'll be able to work partial days when I have chemo so she can pick me up about three or four hours after dropping me off. I've been getting drowsy while driving for a half hour or more to my appointments on in-between weeks, and the doctor said I shouldn't be driving long distances.
I mentioned that I'd had a killer headache earlier this week, one that made the backs of my eyes sore. The doctor prescribed a muscle relaxant, Ativan (Lorazepam) for when they get that bad. But I shouldn't make any plans for a few hours after taking it. Hopefully that won't be necessary.
The nurse asked if the Cytoxan made my nose run while it was being administered. I told her no, but it has been running a lot the past few weeks. I'd thought it was an old ailment returning, but apparently not. I'm glad it will only be temporary.
8:25 p.m. - Tuesday, Feb. 07, 2006
CAT Scan Results
Last Wednesday, the 1st of February, I had my biweekly blood labs at the oncologist's. He said my white blood cell count couldn't be any lower, but my medications should be kicking in within the next couple of days. And that I might be sore, especially my lower back and hips, as my body generated new white blood cells.
Fortunately that didn't happen and at the most I felt a little run down.
I also dropped off my CAT scan films and will hear more about them next Wednesday. After looking at the written report, Dr. K. said the scan showed an improvement of about 40 percent from when we started treatment.
So that means that I'm almost halfway there. Great news!
10:31 p.m. - Friday, Jan. 27, 2006
More after-effects?
Didn't get to bed until around 3:30 or so last night. I overslept this morning - awoke around 1:30 and missed an appointment. I called and rescheduled it.
It felt great to finally get a lot of sleep. I wish I could do it more often.
No more fevers, so that's passed.
My hair stopped falling out around the time of the third treatment. I thought it would make the rest disappear, but it didn't. So it's just really, really, thin, and I trimmed it short. It's not falling out but it's not growing either.
My facial hair grows very slowly now also. I only need to shave twice a week.
I've noticed that my fingernails are very brittle, but they still grow at the same rate. If I try to peel a piece of tape off a box with my thumbnail, the nail will tear. I suppose that's a side effect of the treatment as well.
10:24 p.m. - Thursday, Jan. 26, 2006
The Day After
Didn't get to sleep very much last night. I had a hard time falling asleep again. I had to get up early to wait for the phone company to send someone over to put a new jack in the kitchen.
This morning I had a fever between 99 and 100 degrees, so I took a tequin. I was also feeling a little nauseous so I took a prochlorper.
I felt wiped out all day. I finally got a little rest after dinner for a couple of hours. The fever broke while I was asleep and I felt better.
9:06 p.m. - Wednesday, Jan. 25, 2006
Chemo Round 4
Saw my doctor before starting chemo, and everything looks good. My white blood cell count is back up again. He wrote me a new prescription to deal with the headaches.
I told him my fingertips are usually numb and he said it's from the vincristine. Nothing to worry about unless it starts to get worse, such as not being able to feel change in my pocket.
Thankfully, it was nice and peaceful this time so I didn't have to get out the DVD player. I slept a little after the benedryl but not enough.
It still took five hours, and I felt wiped out again afterwards.
I felt a little nauseous when I got home, so I took a prochlorper and that seemed to help.
I sure am grateful that I don't have to go through this every week like some others do, or even every day in some cases. I consider myself very fortunate.
11:50 p.m. - Tuesday, Jan. 24, 2006
Second CAT scan
Today's CAT scan went better than the last one. The preparation instructions were different - last time I didn't have to do anything.
This time I couldn't have anything to eat three hours prior to the test, and had to drink 40 ounces of water before arriving there. I suppose that's because the last time, I didn't get quite so much of me scanned.
They said they'd fax the results to my doctor within 3-5 days. Hopefully we'll see some improvement.
6:33 p.m. - Friday, Jan. 20, 2006
Mid-session Visit
Went to the oncologist Wednesday to have my blood checked and talk to the doctor.
My white blood cell count was very low, leaving me very susceptible to infections. He didn't do anything for it, so I'm not too concerned.
Everything else was okay. No new side effects, and my sleeping is improving as well as the headaches. I've been feeling pretty good lately.
Last weekend I bought a portable DVD player, so next Wednesday I'll be all set should it become noisy again.
9:44 p.m. - Friday, Jan. 13, 2006
The Lost Thursday
I was totally wiped out by that last chemo treatment. I went to bed at 11 pm Wednesday night and woke up at 9:30 am Thursday morning. I had a bite to eat, took my meds and vitamins, and went back to bed at 10:30. Slept until 3:30 pm.
That's over 15 hours of sleep. When I awoke at 3:30 I was soaked in sweat and sore all over. Must have been a fever that finally broke.
From then on I felt better as time went on, and was back on my feet raring to go at dinnertime.
I didn't sleep too well last night, though. I was up until around 4. Felt like my heart was racing.
But today I'm back on track. I got up at 1100 and haven't fallen asleep all day. Can't remember the last time that happened.
9:27 p.m. - Wednesday, Jan. 11, 2006
3rd Round of Chemo
Today wasn't too bad. Last time I had a huge black mark on my arm from the needle, and it's still a little visible now.
The facility is very comfortable, with two restrooms, a coat closet, reclining chairs, and free coffee and snacks. They try to make your stay as pleasant as possible, under the circumstances.
You come in they take a blood sample. Then you see the doctor, and he asks how you're doing and tells you the results of the blood tests. If you need new prescriptions, you tell him and they'll be waiting for you when you leave.
This visit, he wrote me a script for a CAT scan. I guess we may be nearing the halfway point.
Then you hang up your coat and drop your bag on a chair. I usually pack a book and a magazine and some snacks in my bag. You let the receptionist know the doctor's done with you, and then sit in your chair.
Soon they start an IV and begin giving you your meds.
That's my routine, and this week the treatment lasted about 5 hours again.
Now I'm not one to complain, but it gets a bit noisy sometimes. The first thing they give me is the benadryl and I usually end up drifting off not soon after. But someone usually ends up making enough noise to wake me up somehow.
This week it was a visitor who was talking to someone in a chair not ten feet away. Yet you could hear her clear across the room.
I asked the nurse if they had any earplugs, but they didn't. So I guess I have to go out and buy an MP3 player, portable DVD player, PSP, laptop computer, or something to block out people WHO TALK LOUD AND WON'T STOP!
I just want some peace and quiet while I'm getting massive amounts of medication pumped into my arm. The least visitors could do is show some respect.
Today's treatment lasted around five hours again. I was pretty beat when I got home.
One more positive note: I actually had a day earlier this week where I didn't take any pain medication. No headache all day long. Hope that becomes a trend.
10:39 p.m. - Friday, Jan. 06, 2006
No Worries
Joints felt much better today. No need to call the doctor.
My temperature has been between 98.4 and 98.8 so it looks like the bouts of fever and incapacitating headaches are behind me now.
Shaved my goatee off yesterday because I got tired of the little hairs falling off all over the place. I'm definitely sporting a new look now.
9:33 p.m. - Thursday, Jan. 05, 2006
New Symptoms
I guess my doctor's visit was a day too soon.
Today I had a lot of pain in my lower back and knees. I knew it wasn't the R.A. because a flareup comes on more slowly with different symptoms. And if my sed rate was high, they would have told me. Besides, with the amount of steroids I'm taking a flareup would be impossible.
I dug out my literature on the medications. Both vincristine and neulasta can cause moderate to severe joint pain. So there you have it.
I just took a lot of painkillers today and it was manageable. If the pain doesn't subside tomorrow, then I'll call the doctor.
9:21 p.m. - Wednesday, Jan. 05, 2006
Labs / Oncologist Visit
Saw the oncologist today and had my blood checked. White cell count was a little low.
He asked if I had any other side effects or symptoms, and I said no to all of them. If it weren't for the headaches and insomnia, I'd be doing fine.
10:12 a.m. - Monday, Jan. 02, 2006
Fallout
The worst part right now is the hair. It's ALL over the place. I guess once it's all fallen out I'll be excited just to find one hanging around. Right now I'm worse than a golden retriever in shedding season.
10:10 p.m. - Friday, Dec. 30, 2005
Aftereffects
My head is still buzzing from the medications, and I again feel out of it for a couple of days after treatment. My face isn't beet red the way it was yesterday, though. At least my appetite is good. Nausea hasn't been much of a problem.
8:08 p.m. - Wednesday, Dec. 28, 2005
Second chemo session
Today's treatment lasted about 5 hours, but I think that's because they were so busy and there were fewer nurses working over the holidays. The benadryl knocked me out again but by the time I left I was ready for a milkshake at the mall.
9:05 p.m. - Thursday, Dec. 22, 2005
The Week After
Finally able to get out of bed after 3 days. I had a temperature that ranged from 97 to 101 degrees, and THE worst headache ever. I could just barely tolerate reading. Sandi made me call the doctor, who said it was probably caused by going from 100mg of prednisone for 5 days down to 5mg. He's having me taper off with 50 for a couple of days, then 40, 30, 20, and 10. I feel much better.
10:02 p.m. - Monday, Dec. 19, 2005
Appointments
Had X-rays taken today of my shoulders, hips, and thighs. Among other doctor's appointments, I spent most of the day in waiting rooms. Saw the oncologist in the afternoon. He didn't see anything significant on the X-rays.
He also had the final results from the PET scan. It looks like I have activity in other lymph nodes, but it's hard to tell in some areas. Inflammation from arthritis can also cause the films to light up in those areas. But since it's in the chest and abdomen areas, it's upgraded to a stage 3 or 4.
We'll do another CAT scan after 3 cycles of chemo, and a final PET scan at the end.
8:22 p.m. - Friday, Dec. 16, 2005
Second Day After
Appetite getting back to normal. Feels good to lie down and rest.
The lump on my neck is completely gone. It's amazing.
9:21 p.m. - Thursday, Dec. 15, 2005
The Day After
Only feeling a bit nauseous, but my head feels different and my heart is racing as if I'd had too much caffiene. That's probably from the Cytoxin. Not to mention all the other stuff coursing through my body.
10:14 p.m. - Wednesday, Dec. 14, 2005
Chemotherapy
The results of the PET scan showed some areas in the left shoulder and hips, as well as lymph nodes in the chest and below the diaphragm. That would make it a stage three or four, but we'll wait and see what the final report says. I'll need to get some x-rays.
The bone marrow test was negative - no lymphoma. That's good news.
Had the first chemotherapy session today. I took a lot of notes. The medications used vary slightly from what I originally wrote down.
- Benadryl - antihistamine
- Dexamethazone 20 mg - Anti-inflammatory
- Rituxan 791 mg - anti-cancer drug
- Aloxi - long-acting anti-nausea
- Doxorubicin - "the red devil" another anti-cancer drug
- Neulasta (the only subcutaneous shot) - Reduces risk of infection
- Vincristine - anti-cancer drug
- Cytoxin - anti-cancer drug
For oral meds, I'm taking an Emend tablet once a day for three days starting today for anti-nausea, and 100mg of Prednisone a day for five days starting today.
The nurse explained each drug and its possible side effects. There are certain things I should watch out for and call them about.
Expected side effects are the change in or loss of taste, and my hair will start to fall out in about three weeks. I should still have hair for Christmas, though. A cumulative lack of energy is the most commonly reported side effect. Fevers can be expected about a week after therapy, for three or four days. It shouldn't be a problem unless my temperature reaches 101.
The session started about 9:30am and was over with about 3:30. Once they see you're not having an adverse reaction to the drugs, they can deliver it at an increased rate. Future sessions should take about three or four hours.
8:12 p.m. - Friday, Dec. 09, 2005
Bone Marrow Scan
The Ativan helped relax me before the bone marrow test. That was an interesting experience. Five more needles, but who's counting. It was very uncomfortable and I don't know how these bone marrow donors do it. I guess you do what you have to do.
Sandi asked if I wanted to go home and lie down afterwards, but I was hungry so we went to the mall to grab a bite to eat and do a little Christmas shopping. Plenty of time for lying down later.
9:10 p.m. - Wednesday, Dec. 07, 2005
PET Scan
Had the PET scan today - not a pleasant experience. That was the fourth needle in three days, but that wasn't anything compared to my reaction. They inject you with a radioactive sugary solution and it let it take 45 minutes to get through your system before doing the scan. The solution is attracted to cancerous cells, so those areas are "lit up" on the films.
Of course I fell asleep in the recliner for about 20 minutes, and when I woke up I felt queasy and my heart was racing. I thought it was a normal reaction to having radioactive isotopes injected into me. I didn't feel much different when they did the scan - fell asleep on the table too, with my arms over my head. (I think my primary care doctor is right about the narcolepsy, but I won't find out until February.)
Felt pretty cruddy as I left but went home to lie down. Sandi called and was concerned about how I felt, so she called the PET scan center and they said I should go to the ER because there is no such thing as a reaction to the shot. I thought they were mistaken, but she came home to check on me anyway. When she saw I was okay, just waiting for the effects to wear off, she went back to work.
We should have preliminary results by Wednesday when I see Dr. K. for chemotherapy.
10:32 p.m. - Tuesday, Dec. 06, 2005
Prognosis
Today marked the first visit with my oncologist, Dr. K. He gave us A LOT of information so this will be a long entry. We tried to take as many notes as possible, and he gave us a folder full of information. He also gave us a notebook to keep our notes in for the duration of my treatment.
While we were there he received the results of the biopsy from Boston. The official name is Diffuse Large B-Cell Non-Hodgkin's Lymphoma and he would classify it as stage 2A, intermediate/aggressive. The growth rate is rapid and right now it's confined to above the diaphragm. It only involves one lymph node that we know of, and I don't have fever, night sweats, or weight loss.
He recommends six to eight chemotherapy treatments every other week followed by a dose of radiation. That would be 12 to 16 weeks, which would end sometime in April. I told him that since the cancer was aggressive, I'd like my treatment to be as aggressive as possible; whatever it takes.
He said I should notice a difference right away, shortly after the first treatment. The lump in my neck should reduce in size and the wicked headaches should go away. He's treated many cases similar to mine with success.
We'll probably be able to get rid of all the cancer and it will be considered in remission. With this type of lymphoma, there's a 70% chance that it will be in remission permanently. Meaning I'll never have it again. I like those odds.
He gave me a few prescriptions for oral medications to get filled prior to my first chemo treatment. They're mostly to treat the side effects:
- Gatifloxacin (Tequin) - antibiotic for fever control
- Lorazepan (Ativan) - causes drowsiness
- Prochlorperazine (Prochlorper) - to treat existing nausea
- Aprepitant (Emend) - to prevent nausea (take 1 a day for 3 days starting on day of treatment)
- Prednisone - a corticosteroid immunosuppressant (100mg/day for five days starting the day after treatment)
The chemotherapy will consist of a battery of medications given intravenously. As far as I could understand, they'll consist of the following:
- Cyclophosphamide (Cytoxan)
- Rituximab (Rituxan)
- 5-Fluorouracil (5-FU)
- Doxorubicin (Adriamycin)
I need to schedule a 2D Echo test with a cardiologist to get a baseline reading. Apparently some of the medication can affect the heart or circulatory system.
I also scheduled a bone marrow biopsy on my way out. They need to make sure my marrow is healthy and there are no signs of the cancer in it. I'm to take 2 Ativan tablets 45 minutes prior to the surgery to relax me. I could also take a tablet if I have trouble sleeping at night. Sandi will be driving me to the appointment so that will work out great.
He asked for the name of my primary care doctor, Dr. N., whom I'll be seeing tomorrow for unrelated health issues. And he'll also be in touch with my rheumatologist, Dr. Y., to see if I should stop taking Humira while undergoing chemotherapy treatment. Humira (adalimumab) is another immunosuppressant, a biological response modifier in the DMARD (disease-modifying antirheumatic drug) class. It suppresses overactive immune systems and calms the arthritis. In my case, it's kept it in complete control, similar to remission.All of the chemotherapy drugs are also effective at treating rheumatoid arthritis (RA). So I'm to stop taking the methotrexate, celebrex, and 5mgs of prednisone daily (except when I'm not on the higher dosage).
Dr. K. stated that there is a high number of lymphoma patients who also have RA. Basically RA is when your immune system goes haywire and starts attacking healthy joints. And apparently whenever you have immune system problems, you're of course susceptible to things you normally wouldn't be. There is a possibility that the RA meds may also play a part, but there haven't been enough studies yet.
9:19 p.m. - Thursday, Dec. 01 2005
Diagnosis
Dr. H. removed the stitches today. He didn't have the results from Boston yet, so there wasn't much more he could tell us. When he does receive them, he'll forward them to my oncologist.
He said it was most likely Non-Hodgkin's Lymphoma, which is treatable with chemotherapy and/or radiation. So that's good news.
I have to make an appointment for a PET/CT scan, to see if the cancer is in any of the other lymph glands in my body. They'll inject me with a solution that contains a type of sugar, which tends to collect in cancerous cells. Wherever I have cancer will be lit up on the films. Hopefully it's confined to the one lump in my neck. I don't have any symptoms anywhere else, so that may be a good thing.
10:06 p.m. - Monday, Nov. 28, 2005
Results
Received a phone call at work from Dr. H. The preliminary results show a malignant lymphoma.
A sample from the biopsy was sent to Massachusetts General Hospital. He may have their results back by the time I have my follow-up appointment with him on Thursday, to get my stitches out.
I'm also scheduled to see an oncologist next Tuesday, the 6th of December.
8:29 p.m. - Saturday, Nov. 26, 2005
Top Quotes from Disney World
Top Quote #3:
"Keep your socks on!"
Top Quote #2:
"I told you to go poo earlier!"
And (drum roll, please...)
The Number One Top Quote from Disney World:
"Don't lick the railing!"
And yes, I wore my Wally World t-shirt and yes; one employee actually said she loved it...
8:12 p.m. - Friday, Nov. 18, 2005
Surgical Biopsy
The surgery was at 0830 so we didn't have to be there too early in the morning. Everything went really well. I'm not sure how much was taken out but the lump feels smaller.
I talked to Dr. H. before the surgery and asked him if there would be any benefit to taking out as much as possible. He said there wasn't since there were nerves and muscles in that area.
I also finally spoke to the anesthesiologist, Dr. D., who had left me a message earlier in the week. He called to get my medical history, but I never could reach him. Every time I called he was in surgery.Going under is always so weird. One moment you're wide awake and the next you're waking up in recovery. I thought I'd be groggy and need to sleep or at least rest when I got home but I had plenty of energy through the rest of the day.
They should have the results by the time we return from vacation on the 25th. There are a few post-op instructions - cleaning and lubricating the incision twice a day - but not much, considering. We're taking bandages just in case, to keep it dry or protect it from germs when needed.
9:01 p.m. - Friday, Nov. 11, 2005
Scheduling Surgery
Happy Veterans Day...
Called to schedule the surgery. It will be next Friday, 18 November. I have to call the day before to find out what time I need to be there.
As always, nothing to eat or drink past midnight the night before. I'll be under a general anesthetic. No aspirin or Ibuprofen the day before; only acetaminophen. And I need to have an adult caregiver stay with me for 24 hours following the surgery.
I don't really care to go under the knife the day before I get on a plane to Walt Disney World. But I told Sandi I'd be okay with that - I'll be on Space Mountain with blood shooting out of my neck, I don't care.
There will be some stitches of course, but I'm to leave the incision unbandaged. That should be interesting.
Nothing I can do now execpt wait.
10:24 p.m. - Thursday, Nov. 10, 2005
Meeting the Surgeon
Today Sandi and I met with Dr. H., the ENT surgeon. We learned that the results of the needle biopsy were inconclusive and that I need to schedule a surgical biopsy.
He looked at the CT scan films I brought along. It wasn't good news. The lump was not only on the outside of my neck. It was dumbbell-shaped, going from the lump on the outside, through the neck and up against my throat. [When I get a chance, I'll scan a good snapshot from the CT films and post a link here.]
As a result, it wasn't possible to remove through surgery. There is a major facial nerve in that area and the tumor is just too large.
He said there were two things that could cause a tumor like that - a viral infection, which might be treated with antibiotics, and lymphoma.
Lymphoma, I learned, is a fancy name for cancer. He said there was something along the lines of a 90% chance that it was lymphoma. Since it can't be treated with surgery, that would mean chemotherapy or radiation.
Sandi took it hard, but I'm holding off on worrying about it until I find out more. We'll see what the biopsy says. Dr. H. will be performing it.
A couple of concerns I asked him about: the tumor has grown rapidly, so is there any chance that it might push against my throat and cut off my air supply and/or esophagus?
He said that was highly doubtful. So that's good news.
I also told him that until we did something about the tumor, I COULD NOT spend another night like last night. I'd been awakened by severe pain in my neck and a horrendous headache. He asked what type of pain relief medication worked for me. Sandi and I couldn't recall what they switched me to in the hospital after my knee surgery - oxycodone or hydrocodone. So he prescribed both.
(Now I can recall that they had me on hydrocodone the first day after they took me off morphine. It definitely wasn't working, so they switched me to oxycodone, which helped much more.)
I also found that the oxycodone tends to make me more drowsy, so at least I could take it before bedtime and take the hydrocodone during the day if needed.
He asked if I had any other symptoms from the tumor, and I told him that sometimes the right side of my tongue and/or mouth would go numb. Especially when I have my head/neck at a certain angle, such as sitting up in bed reading. If I change the angle the feeling comes back. He said that's because it was pressing against the facial nerve at those times. It's not painful, just weird.
9:12 p.m. - Monday, Nov. 07, 2005
CT Scan
Had the CT scan today - didn't care too much for that. But at least I didn't have to fast before the test.
I don't like to say negative things about health care professionals, but that small needle hurt more than any I've had in a LONG time. My eyes have never watered from a needle before.
Once it was in, I could feel it pressing against my vein. As the iodine solution entered my bloodstream, I felt a warm sensation spread throughout my body. Overall I guess it took about 20-30 minutes.
Fortunately I was able to take a copy of the films with me when I left. Which is good since I see Dr. H. in three days.
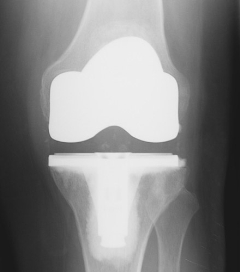
On an unrelated health issue, after the scan I had a follow-up appointment with Dr. B., who performed my total knee replacement surgery this past May. It's now been six months and the knee is doing great. My next appointment is six months from now, at the one-year point.
This is what my new knee looks like:
6:51 p.m. - Friday, Nov. 04, 2005
Initial Visit - Needle Biopsy
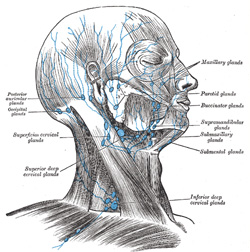
Finally got in to see an ENT specialist, Dr. T. He called it a tumor and said it was probably located in the parotid gland, one of the salivary glands.
I found a good drawing of the lymph glands of the head and neck:
He said it was near a facial nerve and could cause me some problems because of that. It may also cause me to salivate more and/or drool if the tumor causes too much pressure on the gland.
The Mayo Clinic site has a good article on Parotid Gland Tumors.
He decided to do a needle biopsy as a start to analyzing the tumor. After a shot to numb the area, the biopsy wasn't too bad. He then emptied the contents of the needle into a tube with a solution in it. It didn't look like very much came out of the needle but he said believe it or not, they can tell a lot from just a few cells.
If they can't, the next step would be a surgical biopsy. I should hear something about the results in a few days. Dr. T. said I needed to make a follow-up to discuss the results with an ENT surgeon, either Dr. P. or Dr. H.
In the meantime I need to get a CT scan, so on my way out of the building I made the two appointments.
8:56 p.m. - Wednesday, Nov. 02, 2005
A Second Opinion
Today I saw my rheumatologist for my routine semi-annual visit. He actually noticed the lump on my neck and asked if I'd seen anyone about it.
I told him about what my dermatologist had said and he agreed that I should make an ENT appointment. He said if I had a problem getting an appointment that I should call him and he could make some calls for me to be seen by someone right away.
When I returned to work I made an appointment for this Friday. The lump is definitely getting bigger.
5:55 p.m. - Thursday, Sep. 22, 2005
Early detection
I went to see the dermatologist today and asked her to take a look at the lump on my neck. I'd noticed it a couple of weeks ago - it feels like a cyst under the skin or a swollen gland or lymph node.
She measured it at about 3cm across, and it's oval shaped. She said the fact that it wasn't causing me pain was definitely NOT a good sign and that I should have it checked by an ENT doctor.